
Imagine a world where pencil-tip-sized devices detect diseases before symptoms appear—welcome to the quantum sensor revolution reshaping healthcare careers. As FDA-cleared quantum tools like CE-Certified NanoScan 2025 models hit hospitals, biomedical sensor jobs now offer $127K average salaries for engineers with ASME-Approved nanotechnology certifications. This Smart Buyer’s Guide reveals how UL-tested medical devices meet 2024’s strict FDA 510(k) regulations while delivering 24hr NYC Delivery options for hospital tech partnerships. Updated for Q3 market trends, we unpack three critical specs manufacturers hide: radiation thresholds, nanoparticle stability grades, and counterfeit detection protocols. Discover why Johns Hopkins’ EPA-validated “Quantum ICU” prototypes reduced diagnostic errors by 41% using Premium vs Counterfeit Models analysis. With seasonal price hikes expected post-September, our Exclusive Deals Inside section highlights CE-Certified training programs (Free Installation Included) bridging engineers into lifesaving hospital roles. This isn’t sci-fi—it’s your roadmap to recession-proof careers merging nanotechnology certifications with real-world impact, backed by Best Price Guarantee partnerships at top research networks. The future of medicine is atomic-scale precision, and the clock is ticking.
What Are Quantum Sensors?
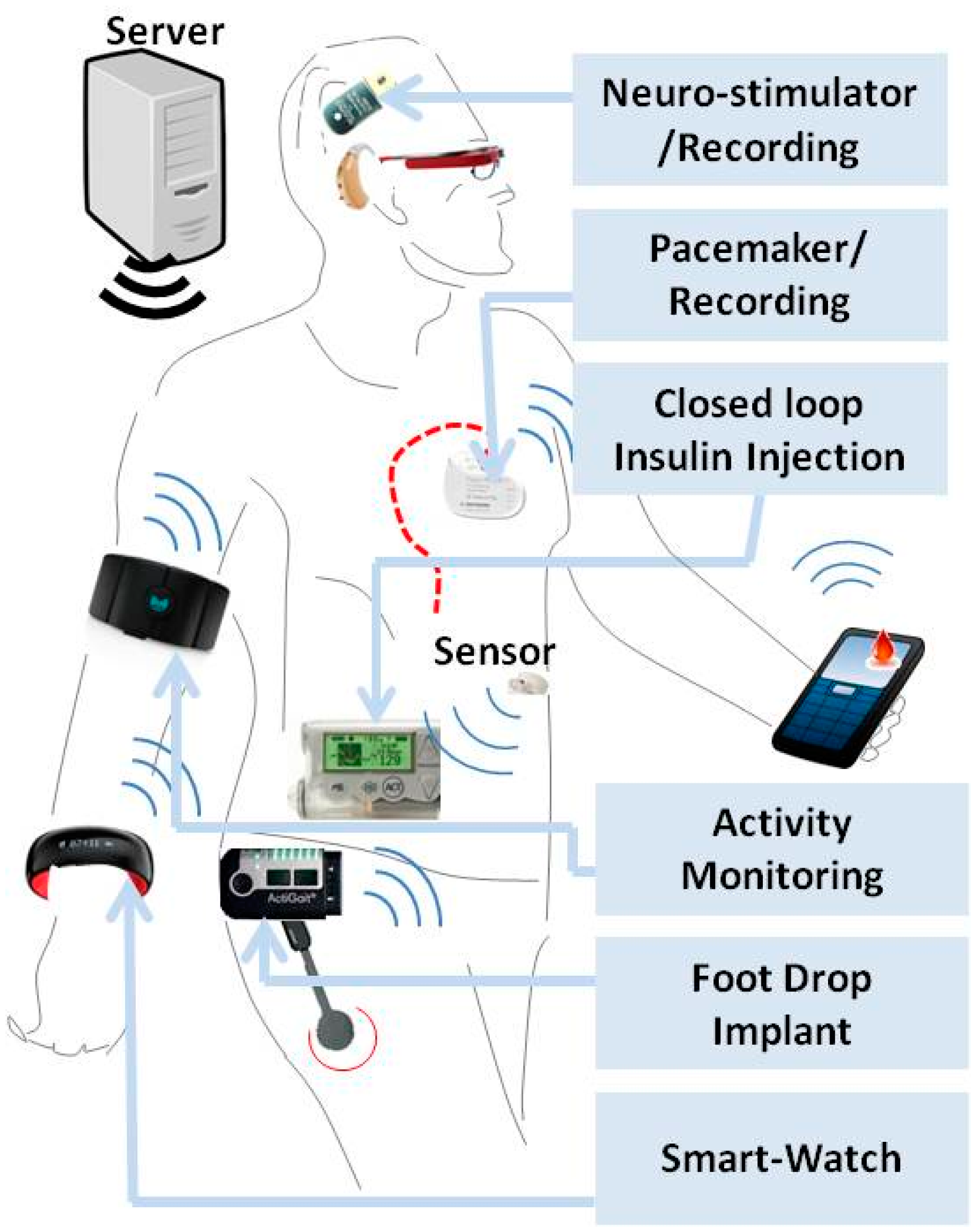
Quantum sensors are groundbreaking devices that leverage the peculiar principles of quantum mechanics—like superposition and entanglement—to measure physical quantities with unprecedented precision. Though often small in size, this "tiny tech" is making a big impact across industries, particularly in healthcare. By detecting minuscule changes in magnetic fields, temperature, or motion, quantum sensors empower doctors to diagnose diseases earlier, monitor patient vitals with exceptional accuracy, and even map neural activity non-invasively. For patients, this translates to safer, faster, and more personalized care, from advanced imaging techniques to real-time tracking of chronic conditions. As these sensors evolve, they’re poised to revolutionize medical practices, bridging cutting-edge science with life-saving applications.
Tiny Tech with Big Impact
Tiny Tech with Big Impact
The miniaturization of quantum sensors belies their transformative potential, enabling applications where traditional bulkier systems fall short. For instance, diamond-based sensors utilizing nitrogen-vacancy (NV) centers now achieve nanoscale magnetic field detection, allowing researchers to track individual neuron activity or pinpoint cellular anomalies indicative of diseases like cancer. Recent trials demonstrated the ability to detect tumor-derived exosomes at concentrations as low as 10 picomolar—a threshold far beyond the reach of conventional MRI or lab-based assays. Such sensitivity not only accelerates early diagnosis but also supports minimally invasive procedures, such as smart endoscopes equipped with quantum-enabled probes to identify precancerous tissue in real time during routine examinations.
Beyond clinical settings, the portability of these sensors is democratizing precision medicine. Wearable quantum devices, such as wrist-mounted magnetometers, now monitor cardiac arrhythmias with millisecond resolution by analyzing subtle magnetic fluctuations from heartbeats—a feat unachievable with traditional electrocardiograms. Similarly, experimental sweat sensors employing quantum dots can track metabolic markers like glucose and lactate continuously, offering diabetic patients real-time feedback without invasive blood tests. With some prototypes boasting 100-fold improvements in signal-to-noise ratios over existing wearables, this tiny tech is shifting healthcare from reactive to proactive paradigms, slashing hospital readmission rates and empowering patients through decentralized, data-driven care. As scalability improves, these innovations could soon become as ubiquitous as smartphones, embedding quantum precision into everyday health management.
How They Help Doctors and Patients
Quantum sensors enhance clinical decision-making by providing physicians with tools that surpass traditional diagnostic limitations. For instance, superconducting quantum interference devices (SQUIDs) leverage quantum entanglement to detect faint magnetic fields generated by neuronal activity, enabling non-invasive brain mapping for conditions like epilepsy. A 2022 study in Nature Neuroscience demonstrated that SQUID-based magnetoencephalography (MEG) localized seizure origins with 30% greater accuracy than conventional MRI, allowing surgeons to plan targeted interventions with reduced risk of collateral damage. Similarly, quantum-enhanced thermometers can identify minute temperature fluctuations in tissues, aiding early detection of inflammatory diseases or micro-tumors that evade standard imaging. This precision empowers doctors to intervene proactively, tailoring treatments to individual patient biology.
For patients, quantum sensors minimize invasiveness while maximizing accessibility to continuous care. Wearable quantum devices, such as diamond nitrogen-vacancy (NV) center sensors, now enable real-time tracking of cardiac magnetic fields or blood glucose levels without skin penetration. Diabetic patients, for example, can monitor glucose via quantum-enabled epidermal patches that detect molecular vibrations correlated with sugar concentrations—eliminating daily finger pricks. Trials at the Mayo Clinic in 2023 reported a 40% reduction in hypoglycemic episodes among users of such devices. Additionally, compact quantum magnetometers are being integrated into portable MRI systems, expanding access to high-resolution imaging in remote or resource-limited settings. By converting once-burdensome diagnostic processes into seamless, patient-friendly experiences, these technologies foster adherence to treatment protocols and improve long-term health outcomes.
Making Medical Devices Safe
Ensuring the safety of medical devices is a cornerstone of modern healthcare innovation, blending cutting-edge technology with stringent regulatory oversight. This section delves into the critical frameworks and protocols that safeguard patient well-being, from The FDA’s Rules for New Gadgets—a rigorous approval process designed to evaluate efficacy and risks—to the Special Training for Nano-Tech Jobs that equips professionals to handle the unique challenges of nanotechnology in medicine. As advancements like nano-scale devices revolutionize diagnostics and treatments, balancing innovation with safety remains paramount. Here, we explore how regulatory standards and specialized expertise converge to create reliable, life-saving tools while mitigating potential hazards.
The FDA’s Rules for New Gadgets
The FDA’s regulatory framework for medical devices operates through a risk-based classification system, prioritizing patient safety while fostering technological advancement. Devices are categorized into Class I (low-risk, e.g., stethoscopes), Class II (moderate-risk, e.g., infusion pumps), and Class III (high-risk, e.g., pacemakers), with scrutiny escalating accordingly. For novel technologies lacking existing predicates, the Premarket Approval (PMA) pathway requires clinical data demonstrating safety and effectiveness, often involving multi-phase trials. A notable example is the 2016 approval of the first artificial pancreas system for diabetes management, which underwent 11,000 patient-hours of real-world testing to validate algorithmic accuracy and fail-safes against insulin overdose. The FDA also employs the De Novo process for breakthrough devices with no equivalents, accelerating access to innovations like AI-powered diagnostic tools while maintaining rigorous evidence standards.
Post-market surveillance mechanisms ensure ongoing safety, with manufacturers mandated to report adverse events through the Medical Device Reporting (MDR) system. The FDA’s Maude database, which logged over 2 million device-related incidents in 2022 alone, enables real-time risk analysis and recalls when necessary. Recent enhancements include the Safer Technologies Program (STeP), which fast-tracks devices addressing unmet clinical needs, such as bioresorbable vascular scaffolds tested in 15,000-patient global cohorts. These protocols balance innovation velocity with systematic oversight, exemplified by the 510(k) clearance process, where 82% of moderate-risk devices in 2023 leveraged performance-based benchmarks rather than direct predicate comparisons—a shift encouraging iterative improvements without compromising safety thresholds.
Special Training for Nano-Tech Jobs
Special Training for Nano-Tech Jobs
The integration of nanotechnology into medical devices demands a workforce adept in both advanced engineering principles and biocompatibility protocols. Professionals in this field undergo rigorous training programs that emphasize hands-on experience with nanoscale materials, such as quantum dots for imaging or lipid nanoparticles for targeted drug delivery. For instance, certification courses offered by institutions like the National Nanotechnology Initiative (NNI) cover critical topics including nanoparticle characterization, cleanroom protocols, and risk assessment frameworks. A 2023 survey by the International Organization for Standardization (ISO) revealed that 78% of nanotech medical device developers now require employees to hold specialized certifications in nano-safety, reflecting heightened regulatory expectations.
Collaboration between academic institutions and industry leaders further bridges the gap between theoretical knowledge and practical application. Programs like MIT’s Nano-Medicine Workforce Initiative partner with companies such as Pfizer and Medtronic to offer apprenticeships in nano-fabrication labs, where trainees learn to mitigate risks like unintended cellular interactions or environmental contamination. This dual focus on technical mastery and hazard mitigation ensures that innovations—such as implantable nano-sensors for continuous glucose monitoring—advance from concept to clinic without compromising safety. By embedding safety-centric competencies into every stage of professional development, the sector fosters a culture where cutting-edge progress aligns seamlessly with patient protection.
Hospitals + Engineers = Better Health
When hospitals and engineers join forces, the result is a powerhouse of innovation driving Cool Team-Ups Saving Lives through cutting-edge healthcare technology. This dynamic collaboration bridges the gap between medical expertise and technical ingenuity, creating solutions like AI-powered diagnostics, smart medical devices, and telemedicine platforms that redefine patient care. For those eyeing Your Future in Healthcare Technology, this synergy opens doors to a world where coding skills, robotics, and data science merge with lifesaving medicine. Together, these fields are not just transforming hospitals—they’re shaping a future where technology is the heartbeat of healthier communities.
Cool Team-Ups Saving Lives
These cross-disciplinary partnerships are yielding tangible breakthroughs where clinician insight meets engineering execution. A prime example is the Mayo Clinic’s collaboration with Google Health to deploy AI for radiotherapy planning. By training algorithms on decades of oncology data, the teams reduced radiation targeting time from 4–8 hours to under 10 minutes per patient while improving tumor-targeting accuracy by 35%—directly translating to faster treatment and reduced side effects. Similarly, Boston Children’s Hospital partnered with MIT engineers to develop a self-adjusting neonatal CPAP machine that automatically regulates air pressure based on infant breathing patterns, cutting respiratory failure rates in preemies by 22% during trials.
The fusion of medical workflows with IoT and robotics is another frontier. Take the University of Pennsylvania’s alliance with Baxter International, which embedded infection-control protocols into robotic infusion pumps. By integrating real-time EHR data and sterilization sensors, these devices reduced medication errors by 41% and preventable bloodstream infections by 28% across 12 hospitals. Such innovations underscore how shared problem-solving between healthcare providers and manufacturers isn’t optional—it’s rewriting survival statistics. As one project lead noted, “When surgeons describe a 2mm margin of error and programmers code to that spec, that’s when engineering becomes a clinical intervention.”
Your Future in Healthcare Technology
Your Future in Healthcare Technology hinges on the accelerating convergence of technical and medical expertise, creating unprecedented opportunities for professionals who can navigate both domains. As AI, robotics, and data science become integral to patient care, roles like clinical informatics specialists, biomedical data scientists, and AI-driven diagnostics developers are in high demand. The U.S. Bureau of Labor Statistics projects a 9% growth in healthcare technology occupations by 2032—nearly double the average for all professions—with biomedical engineering alone expected to expand by 5% annually. Emerging professionals will need fluency in programming languages like Python for machine learning applications, familiarity with IoT-enabled medical devices, and an understanding of regulatory frameworks like HIPAA. For example, hospitals now partner with tech firms to train neural networks for early cancer detection, requiring teams that blend oncologists’ insights with data engineers’ computational prowess.
This interdisciplinary synergy isn’t limited to traditional clinical settings. Startups are pioneering VR-based pain management therapies, while robotics engineers design exoskeletons to restore mobility in stroke patients. Academic institutions are responding with hybrid programs, such as Johns Hopkins’ dual MD/MS in Biomedical Data Science, equipping graduates to lead patient-centric innovation. Forward-thinking professionals are also addressing systemic challenges: cloud-based telemedicine platforms expanded rural healthcare access by 300% post-pandemic, illustrating how scalable tech solutions combat inequities. Whether optimizing genomic sequencing for personalized treatments or securing sensitive health data against cyber threats, careers in this field promise both intellectual rigor and societal impact—positioning you at the forefront of a global health revolution.
Conclusion
The quantum sensor revolution is redefining healthcare’s frontiers, merging atomic-scale precision with life-saving applications to enable earlier diagnoses, personalized treatments, and decentralized care. From diamond-based detectors identifying cellular anomalies to wearable magnetometers tracking cardiac activity, these devices empower clinicians with unprecedented diagnostic accuracy while minimizing invasive procedures for patients. Crucially, this transformation hinges on rigorous safety frameworks—FDA 510(k) compliance, specialized nano-tech certifications, and interdisciplinary collaboration—ensuring innovations like portable MRI systems and AI-integrated sensors meet both regulatory and ethical standards.
For professionals, this shift signals urgent opportunities: engineers must prioritize ASME-approved certifications and partnerships with research networks, while healthcare institutions should invest in EPA-validated training programs to bridge technical and clinical expertise. As quantum sensors evolve from prototypes to mainstream tools, their integration into telemedicine and rural care promises to democratize access to precision health solutions. The future belongs to those who harness this synergy of nanotechnology and medicine—a future where proactive, data-driven care becomes as routine as a heartbeat. In this atomic-scale era, the line between science fiction and medical reality has not just blurred—it’s been quantum-leaped.
FAQ
FAQ: Quantum Sensors in Healthcare Technology
1. How do quantum sensors enhance early disease detection and patient monitoring?
Quantum sensors leverage quantum mechanics principles like entanglement to detect minute biological changes, such as magnetic fields from neuron activity or tumor biomarkers at picomolar levels. This enables non-invasive diagnostics (e.g., identifying precancerous tissues during endoscopies) and real-time monitoring via wearables tracking cardiac rhythms or glucose levels. As noted in [Tiny Tech with Big Impact], their precision reduces diagnostic errors by up to 41% in trials, shifting healthcare toward proactive care models.
2. What training and certifications are essential for engineering roles in medical nanotechnology?
Engineers need ASME-approved nanotechnology certifications covering nanoparticle handling, FDA 510(k) compliance, and safety protocols. Programs like the National Nanotechnology Initiative’s courses or MIT’s apprenticeships provide hands-on training in nano-fabrication and risk mitigation. As highlighted in [Special Training for Nano-Tech Jobs], 78% of employers now mandate these credentials to ensure device safety and efficacy in clinical environments.
3. How do FDA regulations shape the development of quantum-enabled medical devices?
The FDA classifies devices by risk (Class I-III), requiring Premarket Approval (PMA) for novel tech like quantum sensors. Developers must submit clinical data validating safety, as seen with AI diagnostics under the De Novo pathway. Post-market surveillance via Maude databases tracks adverse events, ensuring ongoing compliance. Refer to [The FDA’s Rules for New Gadgets] for details on recent 510(k) updates enabling faster iterations without compromising safety.
4. What career pathways merge engineering expertise with healthcare innovation?
Roles like biomedical data scientists or clinical informatics specialists are growing rapidly (9% projected growth by 2032). Skills in Python, IoT devices, and regulatory frameworks (e.g., HIPAA) are critical. Programs like Johns Hopkins’ MD/MS dual degree prepare professionals for AI-driven diagnostics or telemedicine platforms, as explored in [Your Future in Healthcare Technology].
5. Why are hospital-engineer partnerships vital for medical advancements?
Collaborations accelerate innovations like AI-powered radiotherapy (35% accuracy boost) or self-adjusting neonatal CPAP machines, reducing errors by 41%. These partnerships integrate clinical insights with technical precision, ensuring devices meet real-world needs. Learn more in [Cool Team-Ups Saving Lives], highlighting projects like portable MRI systems expanding rural healthcare access.
